General Information about Malaria, its Symptoms and Appropriate Treatment
A terrible and life-threatening disease such as malaria is not something that people should miss from their sight. Usually, homed in the tropical and subtropical climates, it affects somewhere between 300 and 500 millions of people every year, out of which 1 million of people die. The Centers for Disease Control and Prevention in US report that almost 1,500 cases of malaria appear every year and most of them are developed by the people who travel through the areas where this disease is more common.
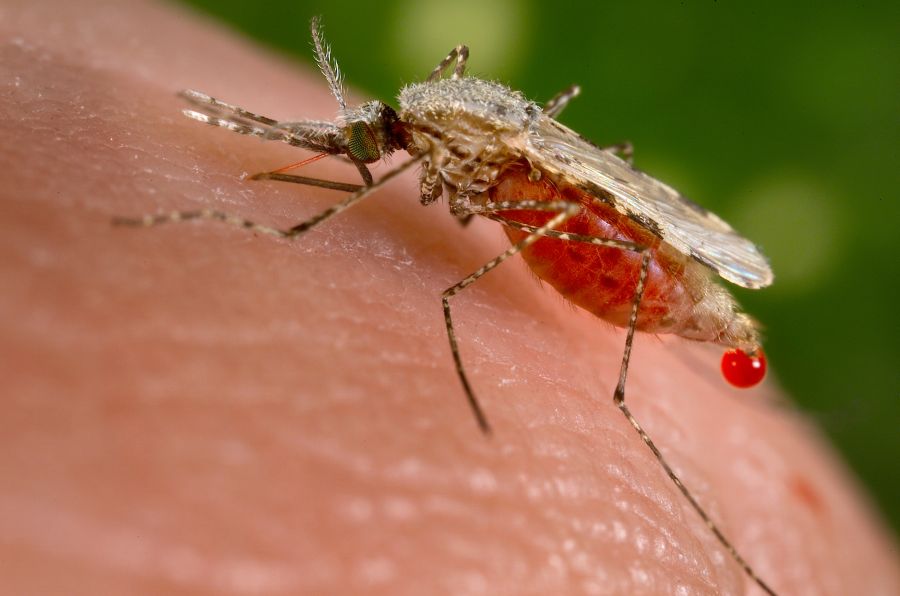
An infected Anopheles mosquito carrying the Plasmodium parasite can trigger the disease through a simple bite. When the parasite is released into the body, it reaches the bloodstream and then travels until it gets into the liver, where it matures. Within only 48 to 72 hours, the parasite located in the red blood cells will multiply, causing the eruption of the infected cells. The infection process continues culminating with symptoms that occur in cycles of two to three days.
Unfortunately, sometimes an infected mother can pass the virus to her unborn child, a fact known as congenital malaria. The disease can also be passed on by making a blood transfusion, an organ transplant or through needles and syringes that have been used before.
Contents
Symptoms:
With a development of 10 to four weeks and sometimes to several months, until the infection asserts, patients can experience:
- Muscle pain
- Nausea
- High fever
- Sweating
- Trembling
- Diarrhea
- Headache
- Anemia
- Bloody stools
- Coma
Diagnostic:
The doctor will begin with some questions regarding your health history and continue with a physical exam that will determine if your liver or spleen are enlarged. If they are, additional blood tests will follow, which will show:
- If you have malaria or not
- The type of malaria
- What kind of parasite is causing it and his resistance to other drugs
- If your vital organs have been affected
- If you have anemia
Complications:
A series of life-threatening complications may arise and end with the death of the patient. Some of these are:
- Destroyed red blood cells that lead to anemia
- Low blood sugar
- The swelling of the brain’s blood vessels
- Amassing of fluid in lungs causing edema
- Organ failure
Treatment:
Based on the type of parasite causing the disease, the doctor will prescribe the right medication. Some parasites are resistant to drugs, which may cause the change of your treatment several times.
Long-Term Overview:
If complications arise, the view on the long term may not be good. In the case of cerebral malaria, brain damage is the typical outcome. Also, if the parasite is resistant to drugs, the disease may re-appear. However, if everything goes well during the treatment, there should be no effects on the long term.
Preventing Malaria:
Considering the fact that no vaccine can prevent malaria, pay a visit to your doctor before going into an area where this disease is common. He will prescribe medicine that usually treat it, but can also prevent it and can be taken during your stay, as well as before and after your return. Also, to avoid mosquito bites, sleep under a net, cover your skin and use sprays which contain DEET.



