What Should Your Blood Pressure Be According To Your Age! Is It High, Low Or Normal?
Every person should measure their blood pressure from time to time and if it’s not within the normal values it should be controlled. High blood pressure is especially dangerous. It can damage the arteries in the heart, lead to heart attack, stroke, heart and kidney failure and many other health hazards. This is what encourages doctors to recommend aggressive therapies in order to keep the blood pressure in line and prevent complications.
The truth is that there is no one-size fits all approach when it comes to blood pressure. What is normal for a 50-year old might not be for an 80-year old and that’s normal. That’s why there are certain guidelines for normal blood pressure according to a person’s age. Doctors have devised the following table in order to give people some orientation regarding their blood pressure. You need to measure it and see which category you fall under. If it’s too low or too high you need to seek some medical attention in order to get it back to normal.
Contents
Blood Pressure Chart By Age
Understanding blood pressure readings is important. Now you may know 120/80 mm Hg is the ideal reading. However, there are various factors that affect the average numbers one should own. For example, age. The normal blood pressure values for children and elderly are not the same. This is a reference for you regarding the normal blood pressure level for 1 month infant to 64 years old elderly.
On the other hand, the blood pressure for pregnant women may fluctuate. But the average level is more or less the same as any adult’s readings. Doctor may determine it as hypertension when the bp result is 140/90 mm Hg or higher.
If you’re unsure about the measuring you can go to your doctor to get an accurate picture of your blood pressure and chart what happens with time. According to the American Heart Association from age 20 and up all people should check their blood pressure at the regular healthcare visit or at least once a year.
It’s astonishing that one in three adults in the US suffers from high blood pressure! And this is the reported number, who knows how many are still undiagnosed. However, a single high reading at the doctor’s office doesn’t necessarily mean you have a condition. It may be influenced by stress, exercise, change in posture etc. But if it stays high in the course of a few days or a month your doctor will probably prescribe a treatment in order to keep it controlled. You’ll need to make some lifestyle changes, start eating healthier, exercising, and probably take some prescription medications.
Don’t wait any longer! Check you pressure right now and see if you need to take some action. Early detection is crucial and can prevent serious complications.
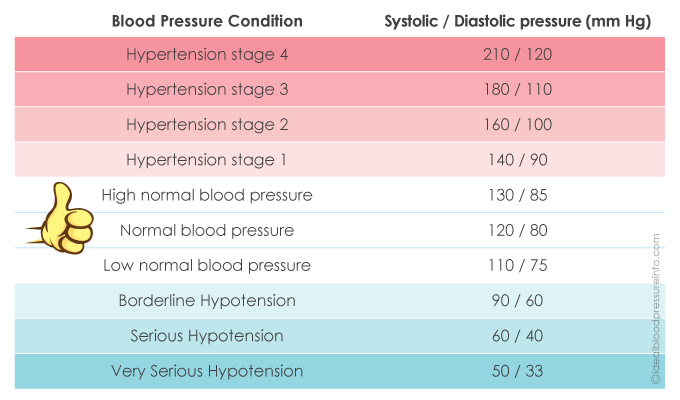
Blood Pressure Reading Chart
Below is a blood pressure reading chart for you.
*Remember that the larger figure in your reading represents the systolic value; the smaller figure represents your diastolic value. Systolic is the measurement of pressure when the heart is beating. Diastolic is the measurement of pressure when the heart is resting.