How to Deal with Pre-menopause without Medicines
Besides menopause, another difficult stage that women have to deal with is pre-menopause. This means that the number of reproductive hormones is decreasing until the woman reaches menopause. This stage lasts between 10 and 15 years.
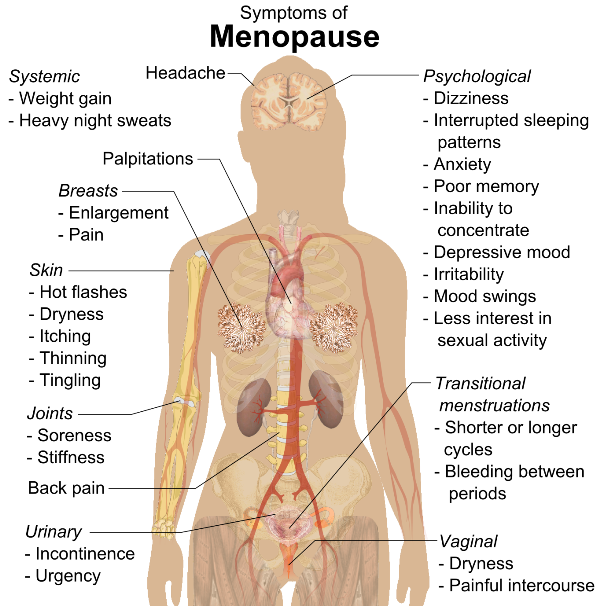
During this period, women experience a broad variety of disturbing symptoms, ranging from mood swings, migraines, insomnia, hot flashes, and heart palpitation to less hair on the legs or underarms. However, even though nowadays you can take a pill for almost anything, the excess of medicines is harmful, and some treatments are not recommended for the long term. What can you do in this situation? You can always rely on Mother Nature and try some natural remedies.
- Soy
Soy is an essential food for any woman who struggles with the pre-menopause stage because it is filled with phytoestrogens. In fact, soy is considered the best source of phytoestrogens. If you want to maintain or reestablish the hormonal balance in your body, you should definitely introduce soy into your diet.
You can eat tofu – which is soy cheese, soy milk, or meals that contain soy flour. For example, muffins and other sweets made of soy flour are both delicious and useful for your hormonal balance.
When a woman is in her pre-menopause stage, she also gets a tendency of gaining weight. This will alarmingly increase the risk of high cholesterol. But soy will also help you keep your cholesterol level under control. Moreover, it has been proven that this super food can also reduce the risk of cancer and heart disease.
- Fruits and Vegetables
Even though eating fruits and vegetables is not a new idea, you should think that at this point you really need to change your diet. In fact, inside your body there are dramatic changes taking place when you are at pre-menopause. They are the reason for all the disturbing symptoms you experience. There is no better way to help your body deal with these changes than making some modifications in your diet. Your body needs essential nutrients to cope with all the issues, and you should provide it these substances by eating raw vegetables and fruits.
If you are switching to a healthier diet, your will notice very soon that you will have a better sleep and fewer mood swings. Moreover, your level of concentration will also be boosted.
Another advantage of consuming vegetables is that your phytoestrogens level will increase. This will happen especially when you eat dark leafy vegetables, such as kale, spinach, collards, turnip greens, broccoli and romaine lettuce. Try to eat this type of vegetables at least once a day and you’ll get rid of frequent hot flashes. Furthermore, your libido will be increased!
What Not to Eat
If you experience the symptoms of pre-menopause, you should avoid foods that are high in sugar, alcohol and caffeine. Red meat is also worsening these symptoms so that you are advised to refrain from it as much as possible.




Soy? All soy is gmo …. won’t touch the stuff.