Top 5 Home Remedies against Keratosis Pilaris
Keratosis Pilaris is a skin condition that brings an unwanted look and itchiness in some areas of the sufferer’s body. The typical look consists of bumps, rough skin, and redness. Besides having an undesirable look, the skin can also become quite itchy.
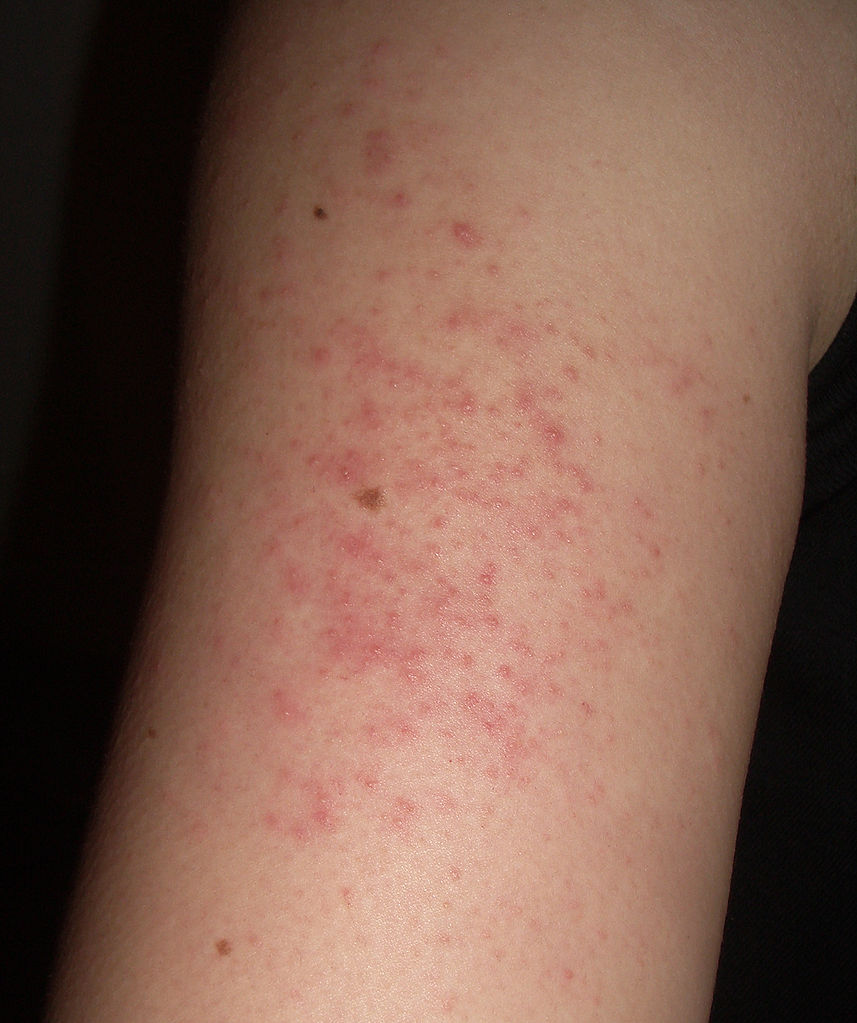
The condition does not pose serious health issues, however, and can be treated using simple ingredients that you can easily have access to during your daily life.
Here is a list of the best remedies for the task:
- Coconut oil
Coconut oil is excellent when it comes to skin problems due to several reasons. First of all, it has strong antibacterial and anti-inflammatory properties that can clear your skin and improve the feeling in the area.
Second of all, it is an excellent moisturizer. Seeing how Keratosis Pilaris often leads to dry skin in the areas affected, it is very indicated in this case as well.
Studies have shown coconut oil to be effective against dry and itchy skin, providing proper nourishment, while killing bacteria responsible for problems such as eczema.
Simply apply a small amount on the affected area regularly, and you should see improvements in time.
- Aloe Vera
This plant is extremely popular when it comes to skin problems, with numerous products incorporating as an ingredient. However, it can be used very well on its own, for best results.
When it comes to Keratosis Pilaris, the gel will make the bumps decrease and moisturize the skin, while allowing the dead skin to be eliminated quicker.
In order to moisturize your skin, reduce your itchiness and exfoliate the area, apply the gel after washing the skin.
- Apple Cider Vinegar
Apple cider vinegar exfoliates the skin and kills bacteria due to its acidic nature. As a result, not only can you fight the cause of this skin condition, but you can also find quick relief from the itchiness.
It is important to dilute it a bit before applying it. Mix it with water, equal amounts of each. Use a cotton ball to absorb some of the liquid and apply it in the area affected. Doing this each day can help you battle the condition effectively.
- Baking soda
This is excellent exfoliator that can be used in various skin conditions. Its ability to regulate the skin’s pH can help create environments that are not suitable for some types of bacteria. Its antibacterial properties also ensure that you do more than find relief from the itchiness and unpleasant look of your skin – you will actually fight the agents that cause the infection in the first place.
- Yogurt
The lactic acid found in yogurt is ideal for dealing with the dry skin that keratosis pilaris causes. Simply mix two teaspoons of yogurt with one teaspoon of brown sugar. Massage it gently into the affected skin, letting it absorb the mixture. Leave it to act for 5-10 minutes and rinse with warm water. Do this three times a week, until you find the improvement desired.
As you can see, there are some simple, yet effective ways of approaching this condition. However, medical advice is still recommended in cases where symptoms persist.




1 comentariu